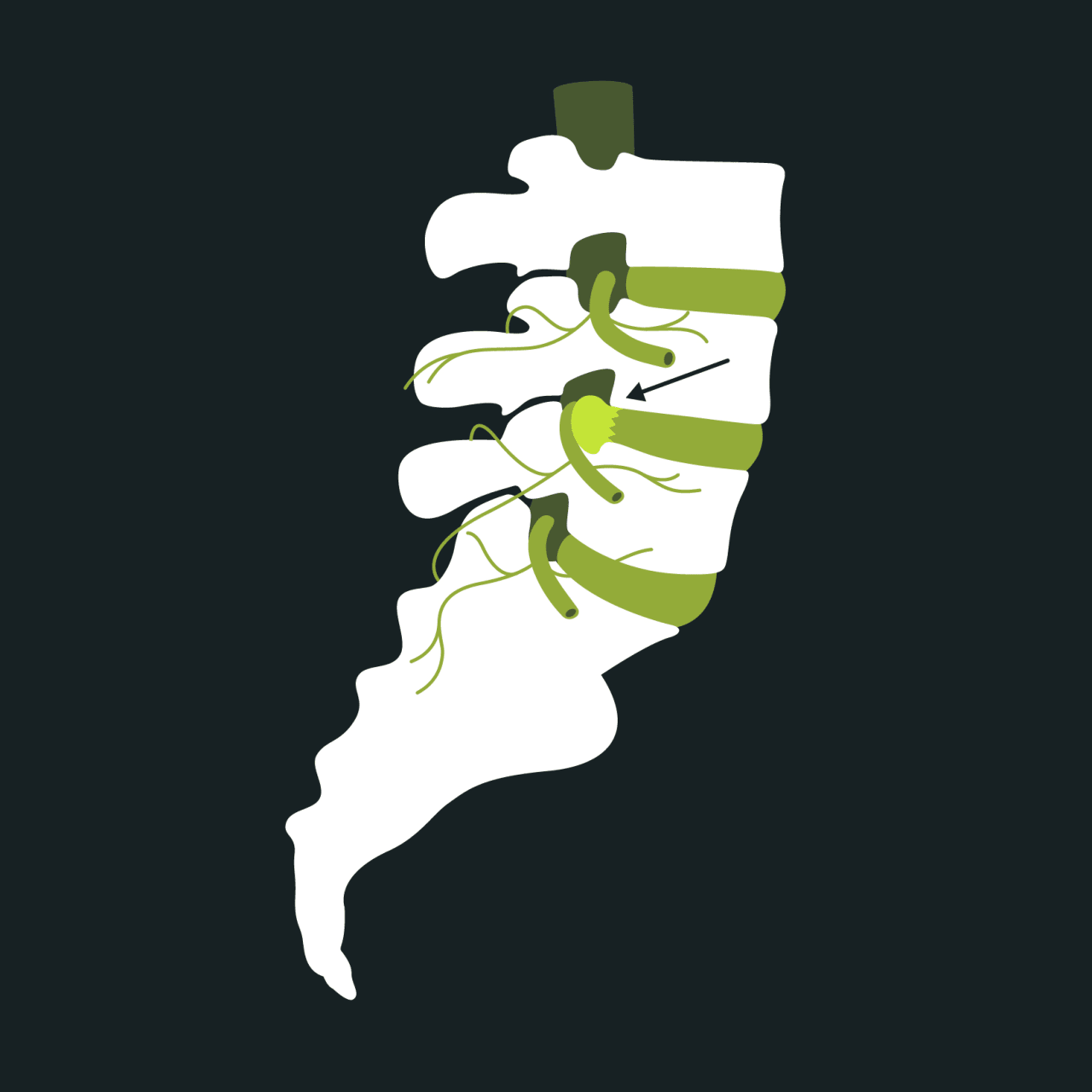
Herniated disc

What are the types of herniated disc? What are some of the causes and symptoms? How can you treat them yourself ?
Your spine is made up of many vertebrae stacked on top of one another. The vertebrae have fibrocartilage (intervertebral discs) in between them to cushion them. These intervertebral discs act as shock absorbers to protect your bones from everyday impacts. If they begin to wear, it can cause pain. Many people say they experience it as discomfort that radiates down to their legs and causes numbness.
01. What is a herniated disc?
02. What are the symptoms of a herniated disc?
The symptoms of a herniated disc vary depending on where in the spine it occurs. If the herniated disc is in your lumbar spine, you’ll usually get severe and sudden back pain. Every movement is excruciating and makes your pain worse. Your body will go into a protective posture, while your muscles will harden and feel stiff. A herniated disc in your cervical spine, is usually accompanied by discomfort in your neck. You’ll often be holding your neck at an angle and be in pain, which might radiate to your arms or the back of your head.
The most common herniated disc symptoms:
- Back pain
- Restricted movement in the affected segment of your spin
- Muscle tightness in the affected area of your spine
- Pain radiating to your legs, arms or neck
- Nerve disorders (disrupted sensations in certain areas of skin)
- Weak muscles
- Signs of paralysis, tingling and numbness
- Lost or impaired reflexes
03. What causes a herniated disc?
Age-related degeneration of intervertebral discs and poor weight distribution on the spine first causes disc bulging (disc protrusion) and ultimately results in a herniated disc. If the spine is angled forward and then rotates, this can cause damage. Lifting heavy loads exacerbates the imbalanced weight distribution on your spine. If you lift drink crates from your car with your legs stretched and your back bent, you’re not doing your back any favors. The shearing forces working in opposite directions start destroying the healthy fibrous rings around your discs. The gel core can then start to leak out.
A herniated disc isn’t always the cause of your pain – that means surgery or injections will only offer slight or temporary relief. But you can reduce the pain by treating the tension imbalances in your muscles and fascia in a targeted way.
«Despite common misconceptions, the herniated disc is not usually the root cause of the problem; it is the painful tightening of the muscle fascia. Here, the right therapeutic support combined with special exercises at home can achieve great results. This should be favored over disc surgery, the benefit of which is usually questionable.» Dr. Torsten Pfitzer, holistic pain therapist and health coach
04. What can help you if you have a herniated disc
Many people say that doctors are too quick to turn to surgery. Yet conservative, targeted treatment can help with a herniated disc and alleviate the pain. This is often much more effective and brings longer-lasting results than surgery.
What’s important for this treatment to work? Your own dedication and time. If you want to become pain-free, the most important things are motivation and patience. This might reassure you: after three months, most patients turn the corner.
Remember: avoid prolonged inactivity, even if moving is uncomfortable for you. Ideally, you should keep going with your everyday activities. Is your pain so severe that you can barely stand it? In that case, medicines to relax your muscles, or heat therapy, can help at the beginning. Talk to your doctor if you think this applies to you.
Many doctors recommend the following pose:

Are you halfway to being pain-free? That means you’re ready to start treating muscle and fascia tightness in your back.
- Help ease muscle and fascia tightness by using myofascial release techniques: If you’re working on specific parts of your body, back pain from a herniated disc might limit this. Myofascial release techniques reduce tension in tissue around the spine, restore balance, and can ease pain. Important to know: work on tightness in your pelvic area, the foundation of your spine. Problems in this area have a negative impact on your back. If you have back pain, most of the time it’s because your hip flexors have shortened and are tight.
- Stretching shortened fascia and muscles (leg and hip muscles, hip flexors): this helps improve myofascial balance if you have shortened abdominal and hip flexor muscles, and overly strained back muscles. Stretching is a good option for easing radiating leg pain if you have a herniated disc. The goal here is to ease pressure on your sciatic nerve and release any points where the nerve is “stuck” or has limited movement, which can help reduce pain.
- Strengthening your core muscles: are you aware of how important strong, balanced core muscles are for a healthy back? If your core muscles are weaker on one side, this puts extra pressure on your spine. And it makes another herniated disc more likely, too.
05. Here´s how you can prevent a herniated disc
If you’re looking for a lasting improvement, you’ll need to make some changes. You ultimately want to get rid of the causes that led to your herniated disc.
- Learn how to look after your back: make sure you keep your back straight when you’re sitting, standing and walking. Don’t sit for too long and take regular breaks to get up and move around. Always lift heavy objects from your legs, not from your lower back. If you need to carry heavy loads, keep them as close to your body as you can.
- Moving is the best medicine for back pain: That’s because the discs do not have any blood vessels. They absorb water and nutrients from the surrounding tissues. But to help them get enough nourishment, you need to move properly. Exercise we recommend: yoga, pilates, walking and swimming. Just don’t overdo it.
- Ease tightness with fascia exercises: by treating fascial adhesions, you can correct tension imbalances.
- Strengthen your core muscles: strong muscles along your spine and strong abdominal muscles will ease pressure from your spinal discs. They work like a natural support (orthosis) to stabilize your spine. Important to know: don’t train your muscles into getting even shorter.
- Watch your weight: people who are of a healthy weight are less prone to herniated discs than people who are overweight.